Lifestyle modification involving adequate physical activity is a cornerstone in the management of diabetes. It complements the effect of the medicines used in the management. There are

There are many types of insulin each working in its own unique manner, some types of insulin are suitable for one but not for another. Normally basal

New insulin delivery devices . LifeScan One Touch Via® This is a super slim pump device which delivers only bolus (rapid acting ) insulin. The cartridge can

You must have been tired listening to doctors mentioning do some exercises …… but not many go into details of how to exercise, which exercises to

It is a welcome change in the climate after months of scorching heat in the middle East. This might last for a couple of months before

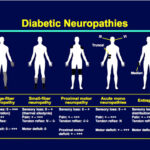
Diabetes is on the rise the world over. Just about anybody can become a diabetic whether you are rich or poor or a male or female
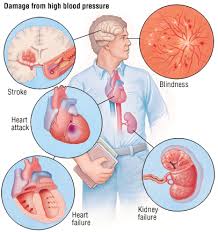
Checking the blood sugar is as common as checking ones blood pressure these days, but is not done as frequently though. There may be no symptoms at

Treadmill is the commonest equipment bought for the home gym and is also one of the commonest equipment used if one frequents the gym. It is often