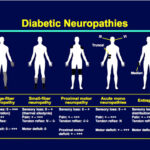
Fasting from dawn to dusk in the holy month of Ramadan for healthy adult Muslims has been ordained and physically sick Muslims are exempt from it.

Normally during the cold winter months, the levels of HbA1C, the 3 month average of sugar, can be higher due to higher food quantity consumed to

Glycemic index ( GI )of a food is the increase in blood glucose ( above fasting glucose) 2 hours after ingestion of a constant amount of food
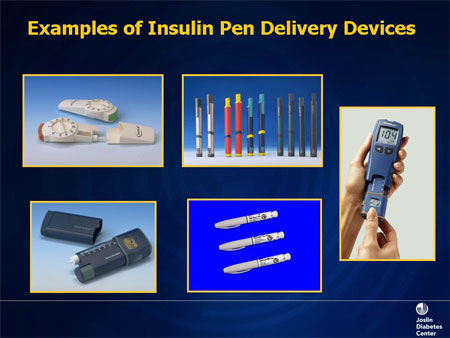
Indications for insulin usage: When oral medicines fail to control the sugar in maximum doses when there are complications to the eyes, kidney or heart, when
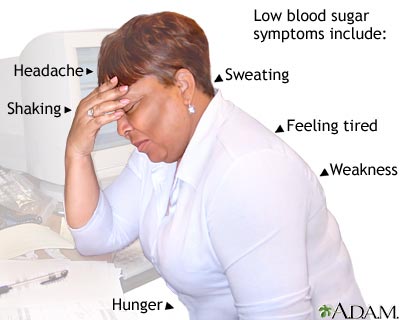
Hypoglycemia or low sugar is one of the nightmares of the patients and the doctors alike. High and low sugars may both present with sweating ,
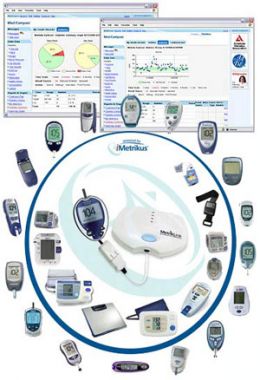
If you have diabetes, one needs a blood glucose meter — a small device — to measure, store and display the blood glucose level. Glucometer is